Common Pitfalls During the CE Marking of a Medical Device or IVD
A CE (Conformitè Europenne) Mark is mandatory for medical devices manufactured, designed, marketed, and supplied within the European Economic Area (EEA) & European Union (EU). The CE Mark is a representation of the manufacturer’s declaration that the product complies with the EU’s applicable directives/regulations.
Compared to the MDD & IVDD, the current MDR 2017/745 & IVDR 2017/746 introduces a life-cycle approach to ongoing CE Marking compliance, and hence it is important to be aware of the most common pitfalls, which if not thought about, may occur at any stage of the lifecycle of a medical device and cost the applicant time and resources.
Elexes has helped several MedTech and IVD firms successfully navigate CE audits and avoid common pitfalls with technical file readiness.
For R&D heads and RA directors, avoiding CE documentation errors saves months and repackaging costs, partner with Elexes for audit-ready technical files.
Common pitfalls during the CE marking
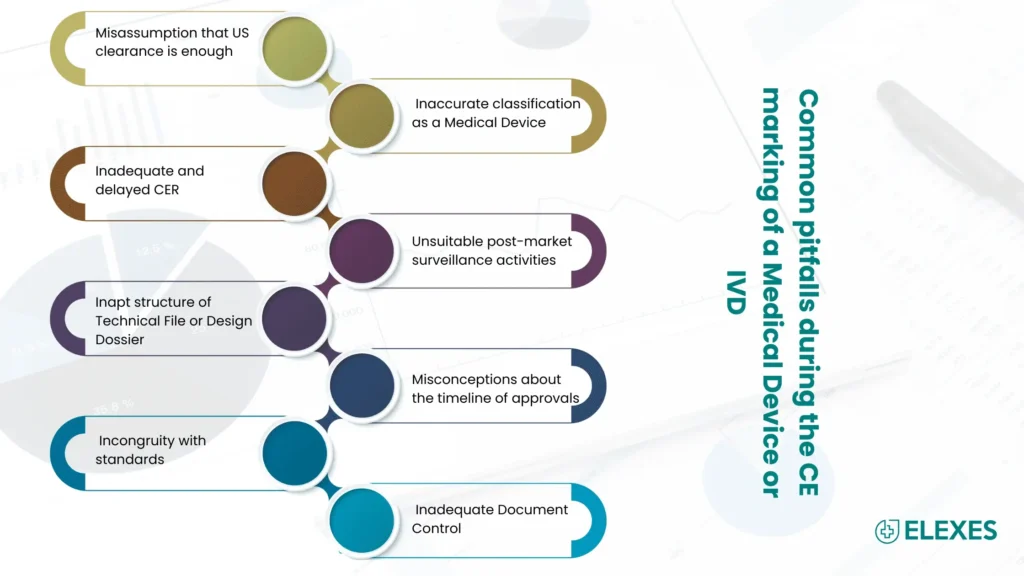
Following are the most commonly observed pitfalls when a medical device company plans to obtain a CE Mark for its medical device or IVD.
⦿ Misassumption that US clearance is enough
Often companies think that the clearance in the US is a doorway to CE Marking in Europe. However, given that in Europe, regulatory approval and supervision are shared by a number of entities, including the Member States, Competent Authorities, and Notified Bodies, the US FDA regulatory approval, if any, will not be considered in the certification process.
To be eligible for the CE Mark, a company’s product must meet the regulatory standards of the EU MDR 2017/745 or EU IVDR 2017/746. Per these regulations, technical files and other technical documentation should be submitted to the Notified Body that you choose to work with.
⦿ Inaccurate classification as a Medical Device
The European Union has its own definition and criteria for a product to be a medical device or an IVD. It is vital that a Manufacturer does the due diligence to precisely conclude if his product is a medical device, a cosmetic, a personal care item, medicine, laboratory equipment, or a consumer product.
The complex regulations and requirements must be understood during this due diligence as some goods are essentially cosmetics, but they can also be used as medical devices due to their implicit medical or clinical application.
Without clearly understanding the applicable directives, exemptions, etc a company should not spend its resources, time, and money in pursuing a CE Mark.
⦿ Incorrect details on outsourced processes
Many licensed manufacturers outsource to contract manufacturers crucial aspects of a product life cycle, such as design, quality testing, production, etc.
The location, scope, quality system certificates, and accreditation of a subcontractor are significant requirements for a CE Mark. The legal manufacturer should ensure that the information about the contract manufacturers is given appropriately as per the requirement of the regulations.
There are possibilities of expired QMS Certificates, no QMS certificate, or legitimate QMS issued for an address other than the manufacturer’s preferred/specified location. All these possibilities should be avoided.
⦿ Inadequate and delayed Clinical Evaluation Report (CER)
Even though a CER has no bearing on the device’s design, if the report’s submission is delayed, the certification may be delayed, as the CER plays an important role in demonstrating the clinical safety or performance of the device.
Although the Clinical Evaluation Report is an important document, its completion is frequently viewed as a regulatory burden and often some important aspects associated with it might be overlooked, like risk management considerations.
For the CER, every manufacturer should determine equivalence according to the guidelines, ensure risk management is considered, and include every piece of information that could be used for supporting the subject device’s safety and performance.
⦿ Unsuitable post-market surveillance activities
Improper post market surveillance (PMS) procedures or unsatisfactory execution of approved activities affect the progress of CE Mark to a vast extent. Manufacturers may have a wide range of devices with varying levels of risk.
The PMS plan followed for these devices might not be sufficient to support a device’s CE marking. Each device or a particular group of devices requires a specific PMS Plan to confirm clinical performance and safety across the predicted lifetime.
The hazards identified in the PMS should be checked with those identified in the risk management file. The link between risk management and PMS is crucial to ensure device certification, yet it’s often overlooked.
⦿ Inapt structure of Technical File or Design Dossier
If the medical device manufacturer fails to submit the technical file or design dossier in the required or expected manner, the CE marking certification procedure may be jeopardized.
The inapt compilation of the technical file or design dossier makes it difficult for the notified body reviewer to access and evaluate information, resulting in an extension of the planned timeline to obtain a CE Mark.
⦿ Misconceptions about the timeline of approvals
Often, quick approval is expected for several device types, irrespective of their mechanism of action, risk classification, or technological characteristics.
For example, for the devices that utilize animal tissues a notified body will seek a lot of information about the animal tissue, including risk management, sourcing, and viral inactivation, while for device-drug combination products, a detailed investigation of the formulation, dosage, and performance of the drug will be required; seldom extending the overall timeline of approval.
⦿ Incongruity with standards
It is a matter of concern when conformity with applicable harmonized and/or latest standards is not demonstrated effectively.
While declaring compliance with standards, the first thing to do is to check if complete compliance which can be demonstrated via strong evidence exists, and check if there are any updates to the standards, so as to ensure compliance with the ‘state of the art’ requirements of the EU MDR.
⦿ Inadequate Document Control
The non-conformities pertaining to the document control system might delay the issue of the QMS certificate further delaying the CE Marking. A few frequently observed non-conformities include:
- Incorrect version referenced either in the procedure or on the production floor
- Improper control of documents of external origin (e.g., Guidance)
- Incorrectly completed change request (missing signatures & dates, incorrect signatories)
- Wrong versions of files shared with Reviewers
While the pitfalls listed here are common ones, this is not an exhaustive list of what can go wrong during the process of CE Marking. Hence, it is wise to take the support of a company like Elexes that has done CE Marking for over 100 devices and continues to support manufacturers in this endeavor.
If you are a manufacturer or part of an organization looking to launch your device in the EU or update your existing technical documentation, please contact us or drop a note today at [email protected]
FAQs
What are the most common CE marking pitfalls for medical devices?
The most common CE pitfalls include incorrect classification, incomplete technical documentation, insufficient clinical data, and failure to address post-market surveillance requirements.
How does misclassification impact CE certification?
Misclassification can lead to wrong conformity routes, audit failures, and product recalls. It affects risk assessment and documentation scope.
What documents are required for a CE technical file?
A CE technical file typically includes device description, intended use, risk analysis, clinical evaluation, PMS plan, labeling, test reports, and manufacturing info.
How can IVD manufacturers avoid delays under IVDR?
By conducting a proper gap analysis, ensuring timely notified body engagement, and updating QMS and documentation per IVDR Annexes.
What support does Elexes offer for CE marking?
Elexes offers expert support with device classification, technical documentation preparation and review, notified body communication, and CE audit readiness services.